Physical Therapists Break Down Plantar Fasciitis


Did you know Plantar Fasciitis affects as many as 2 million Americans every year? That’s a lot of foot pain!
If you’re experiencing foot pain in your heel, the arch, or the ball of your foot, you may have Plantar Fasciitis, one of the most common causes of foot pain.
What is Plantar Fasciitis?
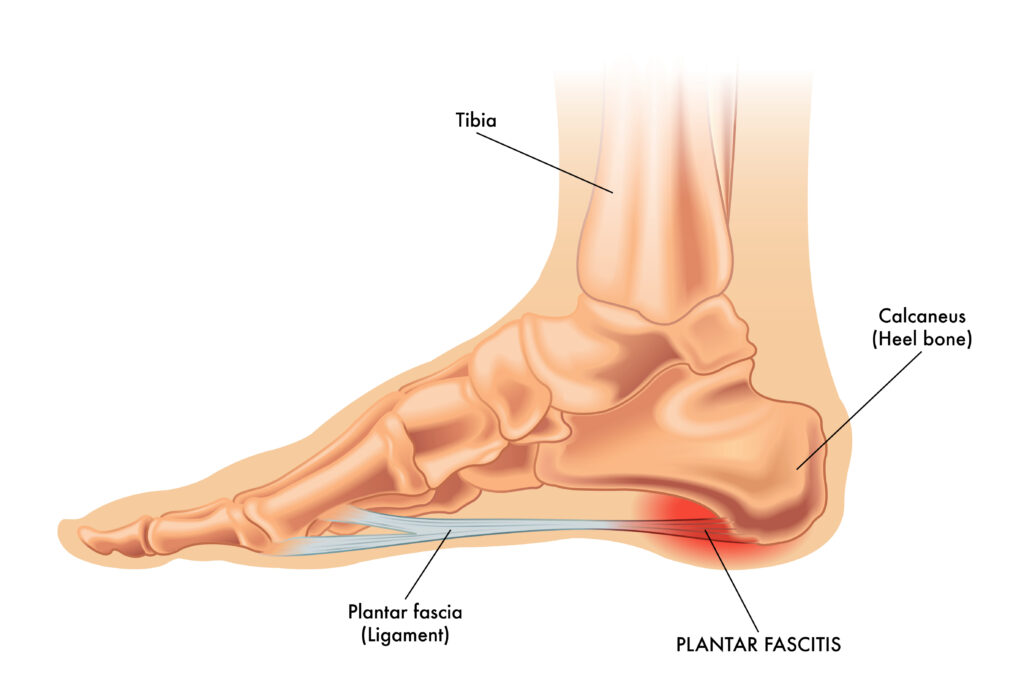

Plantar fasciitis is inflammation of the plantar fascia, which is a strong, fibrous attachment on the bottom of the foot. When the plantar fascia is irritated and swollen from overuse or being overstretched, it causes sharp pain on the bottom of the heel. It’s especially common in runners, people who are on their feet all day, people who don’t wear proper footwear, and people who don’t warm-up properly for exercise. Some health conditions can also increase the risk of plantar fasciitis, including high arches, flat feet, and obesity.
Symptoms Can Include Foot Pain:
- In the morning
- When standing for an extended period
- When standing after sitting for a while
- After activities like running/jumping
- When climbing the stairs
- When walking barefoot
Physical therapists can identify Plantar Fasciitis by massaging, stretching, and pressing on the area to assess pain and mobility limitations.
Physical Therapy Can Help Treat and Prevent Plantar Fasciitis By:
- Assessing and correcting gait/posture
- Strengthening exercises
- Gait training
- Application of ice/heat
- Taping the affected area
- Stretching exercises
- Night splints and other support
- Recommendations for orthotics


A physical therapist will create a customized program based on your needs. They will stretch the Achilles tendon and plantar fascia as well as strengthen the lower leg muscles. They will also be able to assess if your shoes are appropriately supportive enough for you and help you to ease back into activity-pain free.
How to Prevent Plantar Fasciitis:
- Be sure to wear proper, supportive shoes and replace shoes that are worn down
- Wear orthotics or shoe inserts if needed
- Stretch before and after exercise
If you’re already experiencing plantar fasciitis, it can take a few months to feel better. Make an appointment today with a physical therapist who can jumpstart your recovery.