A Century of Progress: Advances in Shoulder Replacement Surgery and What to Expect From Rehab
Did you know that the first joint ever documented to be replaced was the shoulder?
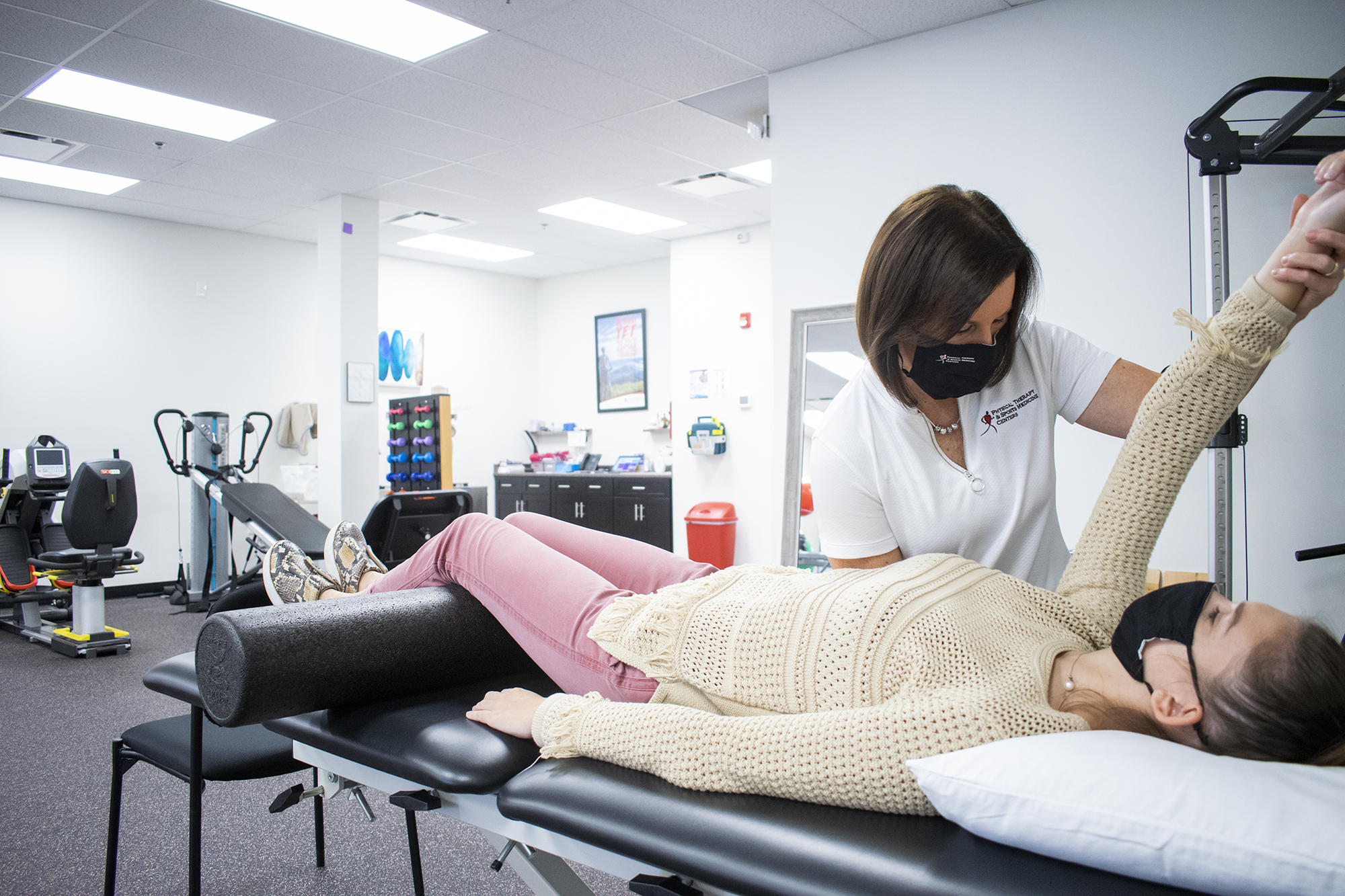
In 1892, Dr. Paen out of France created a prothesis to replace the shoulder of a patient experiencing joint deterioration from a Tuberculosis infection. Thankfully, we no longer have to worry about Tuberculosis, but this innovation was a major medical advance that has transformed significantly over the past 120 years. Although not as popular as a knee or hip replacement, an estimated 65,000 people have shoulder replacements in the US each year.
A shoulder replacement involves removing damaged areas of bone and replacing them with metal and plastic parts to relieve pain, weakness, and stiffness. After surgery, rehab with a licensed physical therapist is essential to restoring function, strength and mobility to the shoulder. Physical therapists and orthopedic surgeons work closely together with their patients to ensure the best possible outcomes – which means, ultimately, a return to activities like tennis and golf without pain.
Recently, PTSMC clinicians met with Dr. Robert Belniak, an orthopedic surgeon who has been practicing for more than 32 years, most recently with Starling Physicians. Specifically, he shared his expertise as one of the few providers specializing and focused on treating patients requiring two different types of surgery: Total Shoulder Arthroplasty (TSA) and Reverse Total Shoulder Arthroplasty (Reverse TSA).

Total Shoulder Arthroplasty (TSA) vs. Reverse Total Shoulder Arthroplasty (Reverse TSA)
The shoulder joint is a ball (humeral head) and socket (part of the shoulder blade) joint. A Total Shoulder Arthroplasty involves the surgeon replacing the ball portion with a metal ball and the socket with a plastic piece. In 1985, the Reverse Total Shoulder Arthroplasty was created – again, in France – by Dr. Gremont. The United States adopted the idea in 2004, and it has now become a major component of upper extremity joint replacement. In the Reverse Total Shoulder Arthroplasty, the ball is replaced on the socket side of the joint, “reversing” the natural structure of the joint.
A standard TSA is best for patients whose muscles and tendons around the shoulder joint are still intact and functioning. If the rotator cuff is damaged, a patient might be a better candidate for a Reverse TSA.
Dr. Belniak spoke to PTSMC clinicians about the differences between the TSA and the Reverse TSA. The Reverse TSA has less overall precautions and a fairly liberal approach in treatment.
Some of the reasons surgeons generally look to avoid a Reverse TSA include:
- Unknowingness behind the replacement’s longevity
- Unpredictability for 100% successful outcomes
- There is no “reversing a reverse,” so the anatomical approach is sometimes the “safer” option
- A patient being younger than 65 years old (Reverse TSAs are typically not recommended for younger patients)
- Rotator cuff being fully intact (including the subscapularis)
- No signs of posterior subluxation (dislocation) of humeral head on glenoid, which poses a risk for success in rehabilitation with a standard TSA

What should I expect in my rehab for shoulder surgery?
Physical therapists are the movement experts responsible for restoring function and mobility post-surgery, and so it’s vital that the treating physical therapist knows and understands which surgical procedure was undertaken, whether the TSA or the Reverse TSA, in order to appropriately treat the patient. Physical therapy typically begins two to four weeks after surgery and focuses on safely building strength and mobility without endangering the replaced joint.
One muscle that physical therapists must pay special attention to is the subscapularis. The subscapularis is a rotator cuff muscle that acts as a major internal rotator for the shoulder and rotator cuff stabilizer. Especially with the standard TSA, the subscapularis – although intact – is removed from an insertional point on the the humerus, which can potentially damage the muscle. Given the “injury” now to the subscapularis, within the rehabilitation process it is crucial to avoid excessive external rotation and extension, as this leaves the shoulder (and the success of the replacement) most vulnerable.
Patients will be restricted in their movements, and will have to avoid lifting anything more than a few pounds, as directed by their PT. After three months, patients should see an increase in range of motion and decrease in pain, and most patients need about six months of therapy to regain pre-surgery function, mobility, and strength. Of course, each patient’s needs and timelines will be different – if you have questions or would like to learn more, contact one of our clinical locations across the state!